Coviu Supports a Telehealth Project for Young Onset Dementia
Young-onset dementia (YOD) refers to anyone under the age of 65 who has been diagnosed with a progressive decline in their mental functioning. Although there are a wide range of illnesses included in the definition of dementia, common symptoms include loss of memory, rationality, social skills and normal emotional reactions. Recent figures suggest roughly 26 000 Australians are affected by YOD, which is roughly 10% of all people diagnosed with dementia.
Life expectancy from the onset of symptoms is extremely short, ranging from 1.3 to 7.9 years. Patients tend to experience a rapid increase in the severity of symptoms and decline in health compared to those who develop symptoms later in life.
One of the biggest challenges for patients is actually receiving a diagnosis, which routinely occurs 5 years after first experiencing symptoms. This is because most medical professionals simply don't consider dementia to be a factor for younger Australians. Once diagnosed, patients often have very few quality years left, which are spent navigating hurdles such as caring for young children, dealing with financial obligations, and navigating grief.
To make matters worse, patients in rural and remote areas have very little access to YOD specialists and support services.
‘It costs an average of $631 one-way for a person who lives more than 100 km from hospital to attend the (Neuropsychiatry) clinic, including lost opportunity costs.’- Dr Wendy Kelso, clinical neuropsychologist at the Royal Melbourne Hospital.
The ‘Bridging gaps in health using telepsychiatry for young-onset dementia’ project is an 18-month project designed to improve access to diagnostics and care for YOD sufferers living in rural and remote regions, whilst simultaneously reducing costs.
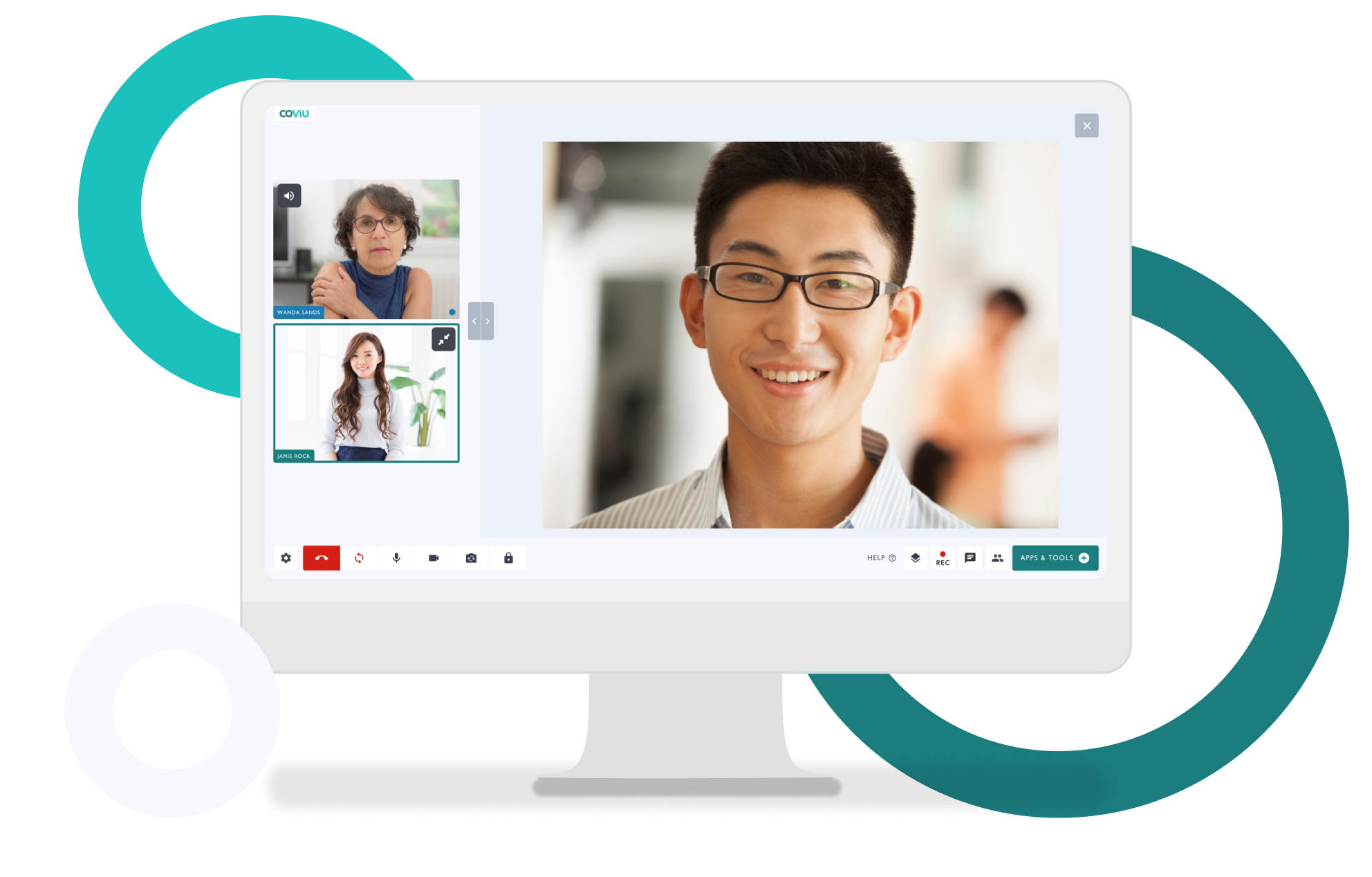
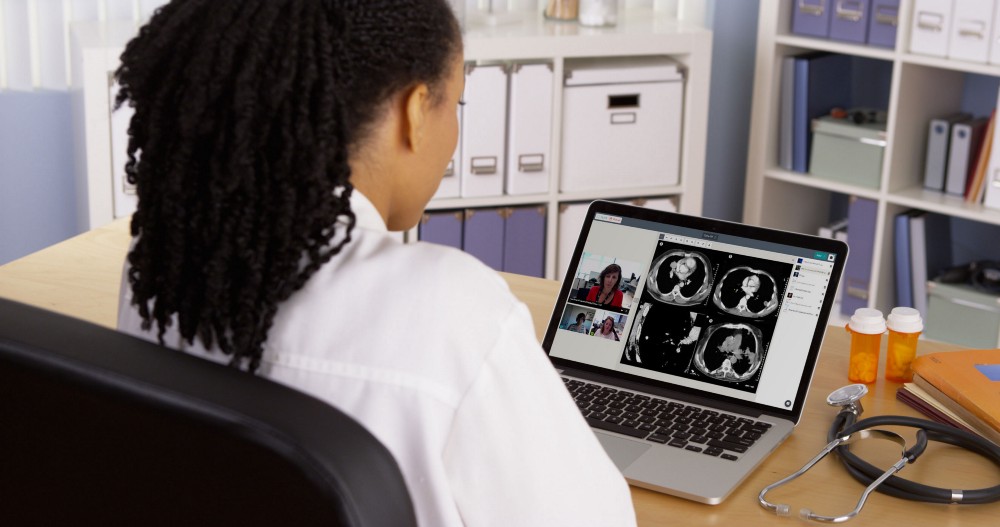
It aims to enhance referral pathways between organisations and increase the use of video consultations to remove barriers to treatment and assessment. The project is using Healthdirect's Video Call service, which is powered by Coviu's browser-based telehealth software.
As of June 3rd this year, the project had been running for 2 months and had held 37 video appointments, saving 16,000 km in travel for clients and their families and over 4.5 tonnes of carbon emissions.
We are so proud to be a part of this amazing initiative, and seeing such great results in a short period of time is very promising. It provides just a taste of what telehealth is capable of once implemented on a nation-wide, or even global, scale.
Find out more about Coviu's telehealth software and how you can grow your practice here.